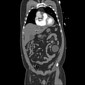
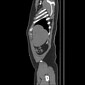
CT - CT Angiography Chest Abdomen
What are the specific complications of Stanford type A dissection in this case?
Haemopericardium resulting in cardiac tamponade. Haemorrhage into the shared aortopulmonary sheath causing stenosis of the (lower pressure) pulmonary arteries.
Aortic dissection with an entry point in the aortic arch. Dissection extends in a retrograde direction to the aortic root and an antegrade direction through the descending thoracic and abdominal aorta with the false lumen continuing into the left internal iliac artery. The left and right coronary arteries emanate from the smaller true lumen and are well opacified. The true lumen supplies the right common carotid artery and the left common carotid artery. The dissected true and false lumina extend through the visualized portion of the left subclavian artery and left vertebral artery. The true lumen supplies the right subclavian artery and right vertebral artery.
The dissection occupies the left lateral aspect of the thoracic aorta before curving posteriorly through the abdominal aorta. The true lumen supplies the celiac trunk, SMA, right renal artery, IMA, left external iliac, and, right common, external/internal iliac artery.
The false lumen extends into the proximal left renal artery however there is good opacification in the mid to distal renal artery indicating communication with the true lumen. There is only mildly reduced renal parenchymal enhancement. The false lumen supplies all the resolvable lumbar arteries, the posterior aspect of the left common iliac artery and the left internal iliac artery.
Relatively hyperdense hematoma (59 HU) surrounds the pulmonary trunk and left and right proximal pulmonary arteries causing moderate to severe bilateral proximal pulmonary artery stenosis. Mild fat stranding in the perivascular mediastinum. Small hemopericardium.